BluePearl Pet Hospital in Monterey County.
BluePearl Pet Hospital in Monterey is located on the Monterey Peninsula in Del Ray Oaks, CA. We serve patients, clients and primary veterinarians from San Luis Obispo to Santa Cruz to Monterey counties and beyond.
Our services.

When your pet needs emergency care, seconds count. Our team is ready to provide expert care 24/7 in case of a pet emergency. If your pet requires a veterinary specialist, we are ready for that too. Our experienced team of veterinarians, vet technicians and support staff work closely together to provide the comprehensive, compassionate care your pet needs and deserves.
The expert veterinarians and staff at our hospital are trained to handle emergencies 24 hours a day, 7 days a week, 365 days a year. Our emergency service provides care for patients that require immediate medical attention, intensive care and hospitalization and/or emergency surgical intervention. We’re here to provide the top level of care for every pet that walks through our doors.
In an emergency, please call ahead and let us know you’re coming. There is no appointment necessary for your emergency vet visit.
At BluePearl Pet Hospital in Monterey, we provide advanced medical and surgical services for ill and injured pets. Our team of board-certified specialists and specialty clinicians are highly skilled and committed to providing your pet with the best medical care.
Through every step of your pet’s specialty care process, we communicate closely with both you and your pet’s primary veterinarian. Your pet’s quality of life is our top priority.
Our
veterinarians.
Caring for your pets is our passion. Meet our team of veterinary specialists here to help you and your pet.
About BluePearl Pet Hospital Monterey.
Formerly known as Pet Specialists of Monterey, our 10,000 square-foot hospital uses the latest and most advanced equipment to provide top-notch care for your pet. Our hospital is equipped with the following special features:
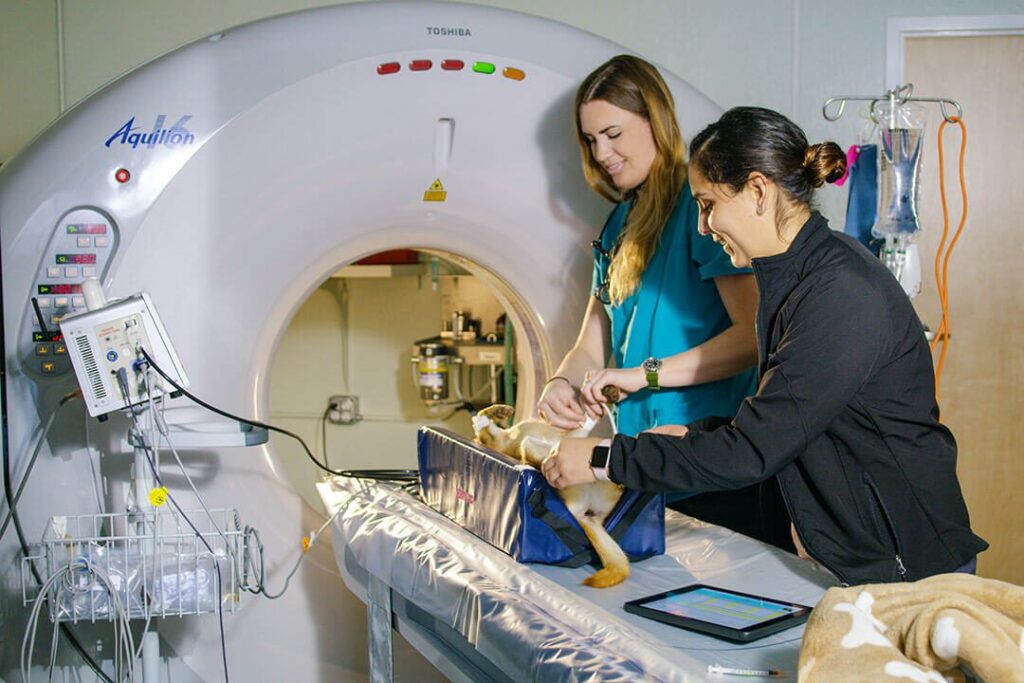
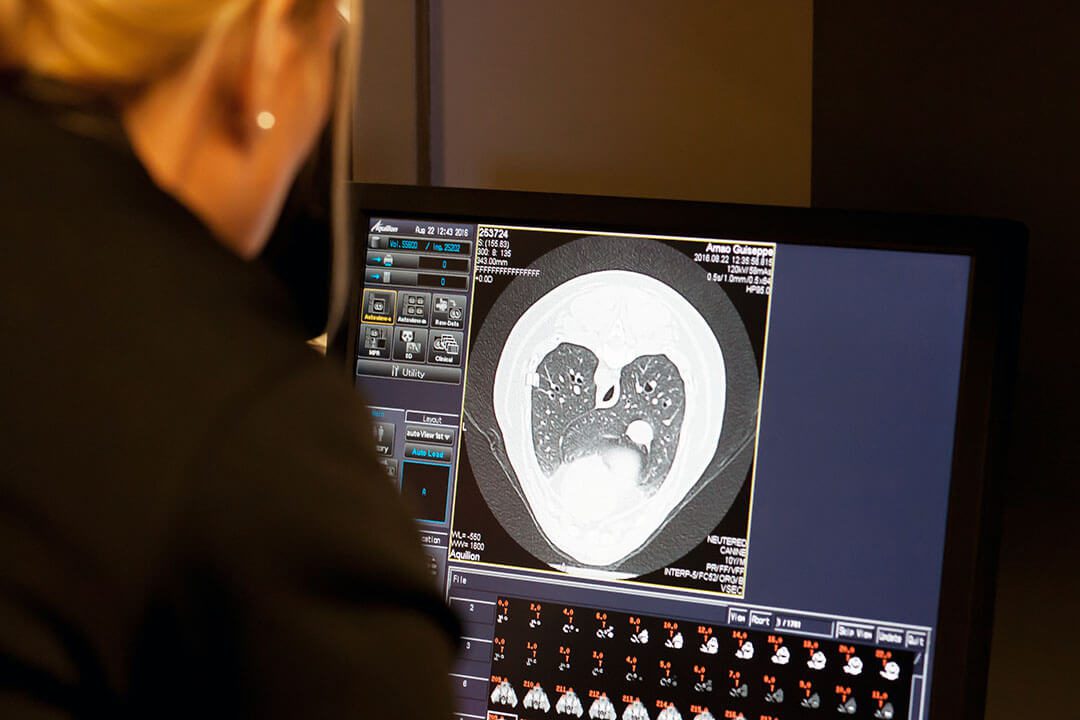
- Diagnostic imaging technology – including CT, ultrasound, diagnostic procedures and in-house laboratory
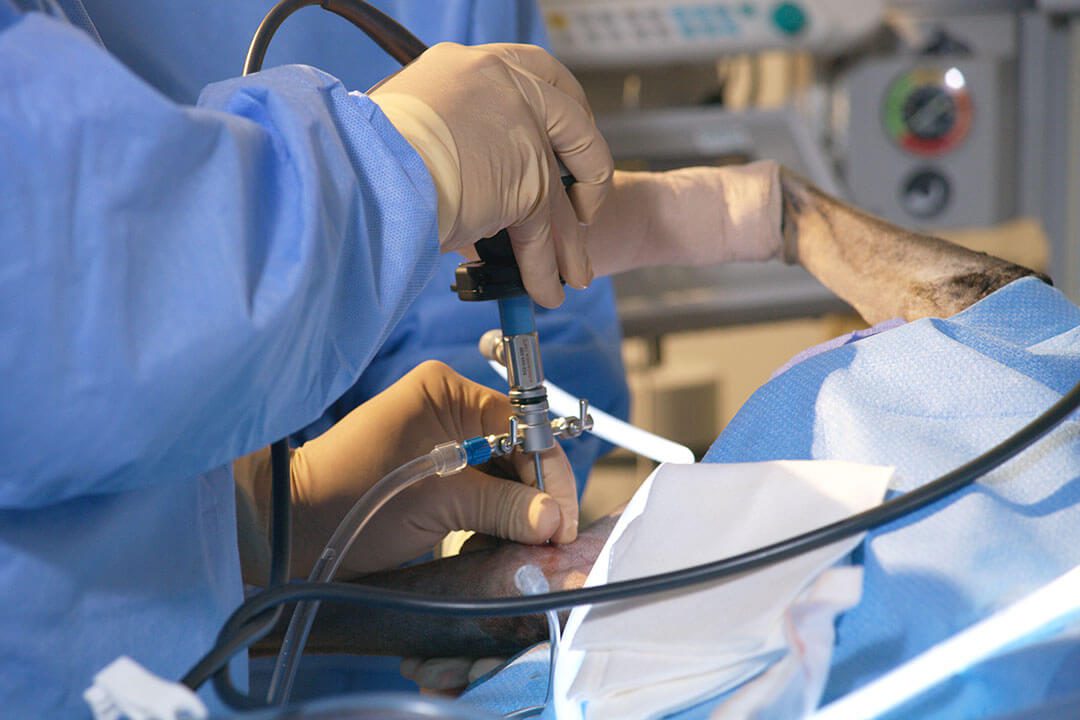
- Surgical suite – with advanced monitoring technology and surgical tools
Emergency history.
Pet owners.
At BluePearl Pet Hospitals, providing our customers with remarkable service is a top priority. We’re committed to making your veterinary visit as smooth as possible.
Have questions prior to your visit? We’re happy to help. Contact our hospital team at 831.899.4838 or [email protected].